
Cystitis is inflammation of the bladder most often caused by infection. Cystitis is the most common type of urinary tract infection

Pyelonephritis is inflammation of one or both kidneys, most often caused by an infection. These are much less common than cystitis
An uncomplicated urinary tract infection (UTI) – Upper or lower UTI in healthy, nonpregnant women with no history of abnormal urinary tract anatomy or function or comorbidities. Uncomplicated UTIs are the most common types.


A complicated urinary tract infection (UTI) – Upper or lower UTI in all other patients.
These generally require more specialised treatment and closer clinical monitoring.
Recurrent UTIs are very common. Approximately 20–30% of women with a UTI will have a second UTI within 6 months.1
Recurrent UTIs can be very debilitating. Living with the the anxiety of sudden infections can negatively impact a persons wellbeing and quality of life
For many people suffering with recurrent UTIs, a prophylactic approach to management may help to minimise recurrences. Contact your healthcare professional who will be able to advise on the most appropriate treatment options for your needs.



Frequent sexual
activity

Use of certain types of birth control (i.e. spermicides)

Hormonal changes due to menopause

Pregnancy

Physical anatomy and hygiene after urination
Antibiotics altering normal bacterial flora

Change in the
immune system

Interference with
urine flow

Prolonged use of bladder catheters
Sexually active women tend to have more UTIs than women who are not sexually active. Having a new sexual partner may also increase the risk to UTIs.
Spermicide-based contraceptives such as coated condoms, diaphragms and cervical caps can be a risk factor for recurrent UTIs.
The decline in oestrogen levels in menopause causes several changes of the normal female physiology and leads to vaginal atrophy, modification of the normal vaginal flora an increase of the vaginal ph. All of these menopause induced changes are associated with an increased risk of developing UTIs in women.
The increased risk of developing UTI’s during pregnancy are related to the increased pressure of the enlarged uterus on the urinary tract, impacting urine flow and bladder emptying. Hormonal changes during pregnancy also increase the risk.
Wiping from front to back after urinating and after a bowel movement helps prevent bacteria in the anal region from spreading to the vagina and urethra.
Our natural bacterial flora are an important defence mechanism against urinary tract infections. Antibiotics can have a negative effect on this flora and increase the risk of developing a UTI.
A suppressed immune system can impact a person’s natural defence mechanisms, making them more susceptible to infection.
Abnormalities in the urinary tract can impair urine flow.
People who are unable to urinate on their own and use a tube (catheter) to urinate have an increased risk of UTIs. This may include people who are hospitalised and people with neurological problems that make it difficult to control their ability to urinate.
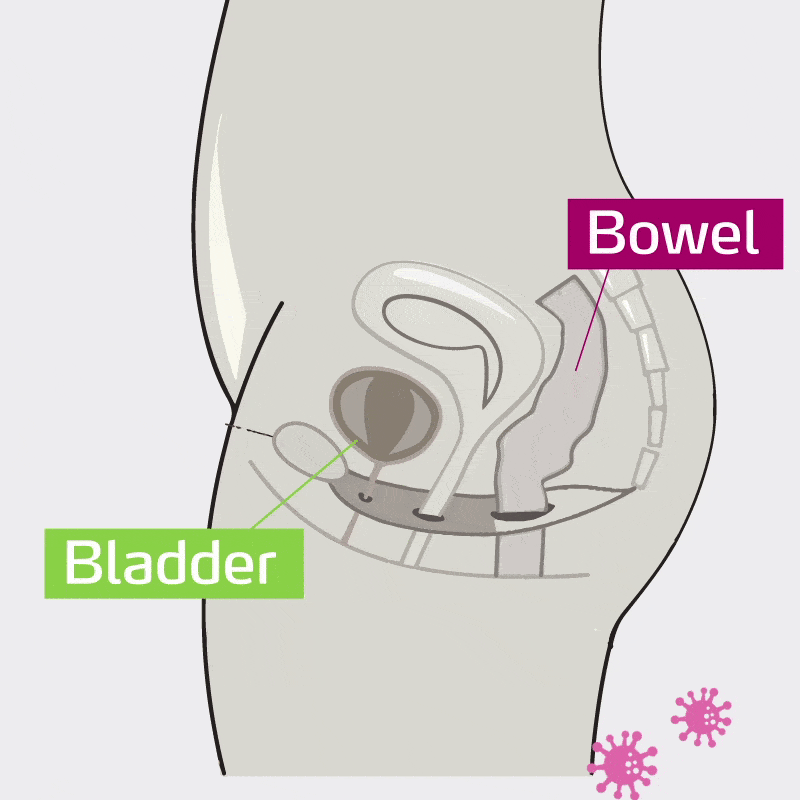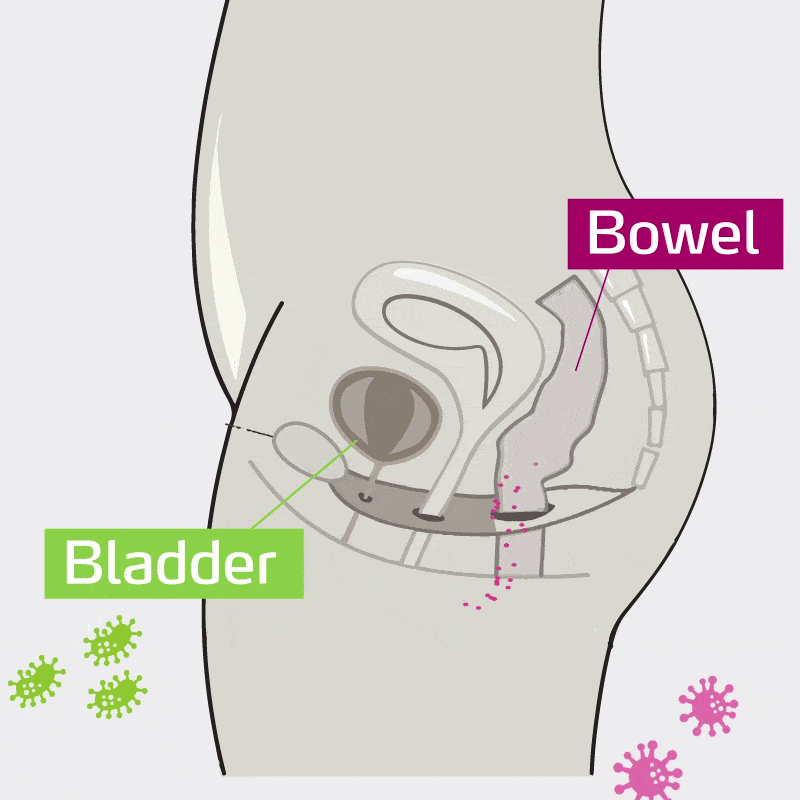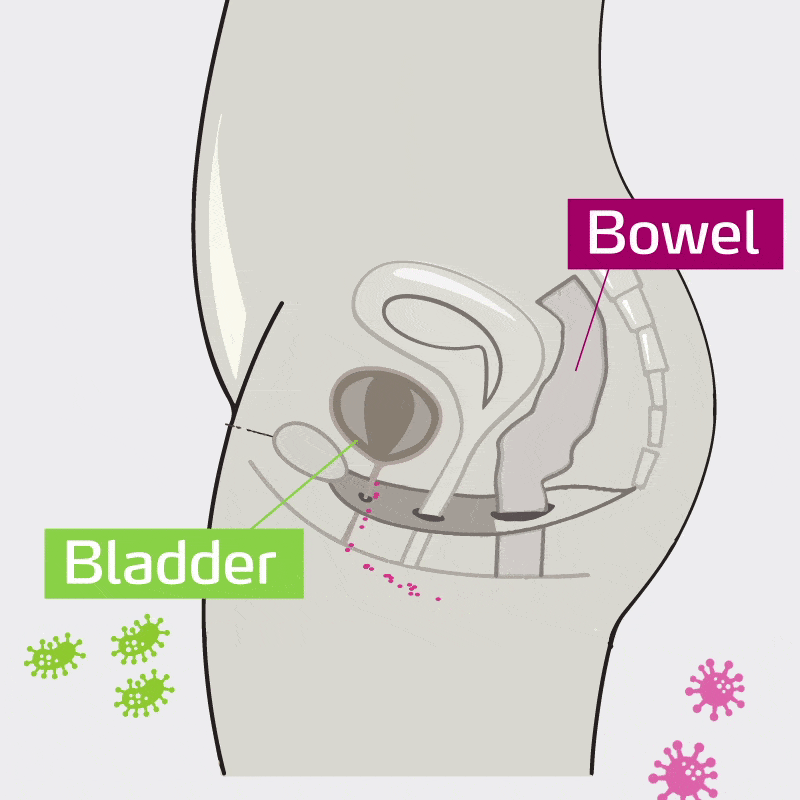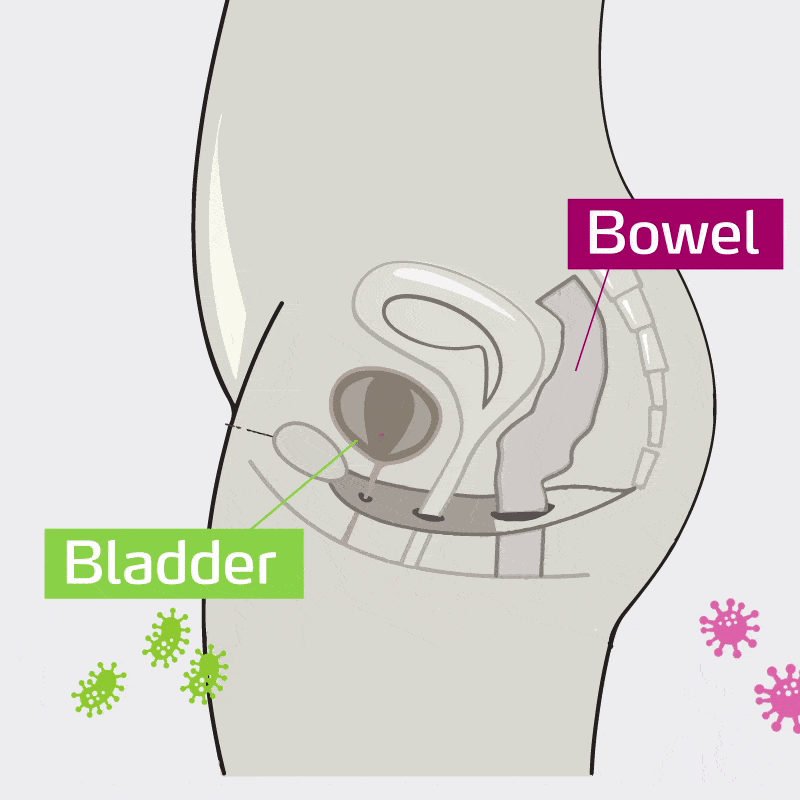
UTI’s are most often caused by certain bacteria in the intestine (Ecoli and other gram negative bacteria) that make their way into the urinary tract.
This makes the intestine an important target for the prevention of recurrent infections.
UTIs are classified as either uncomplicated or complicated infections.
This influences the types of management required.

Utipro Plus AF is
Distributed in Ireland by
Pamex Limited, 100% Irish Owned
Moneen Business Park
Castlebar, Co. Mayo
F23 RX24, Ireland
Tel: + 353 94 9024000

Manufactured by
Noventure S.L.
Avda. Diagonal 549, 5ª planta
08029 Barcelona,
Spain
CE 0476
Copyright © 2022 | Pamex Limited | All Rights Reserved